Health
Breaking down the Malaria Vaccine Rollout in Uganda
The malaria vaccine will be integrated into Uganda’s routine immunization program starting in April 2025.
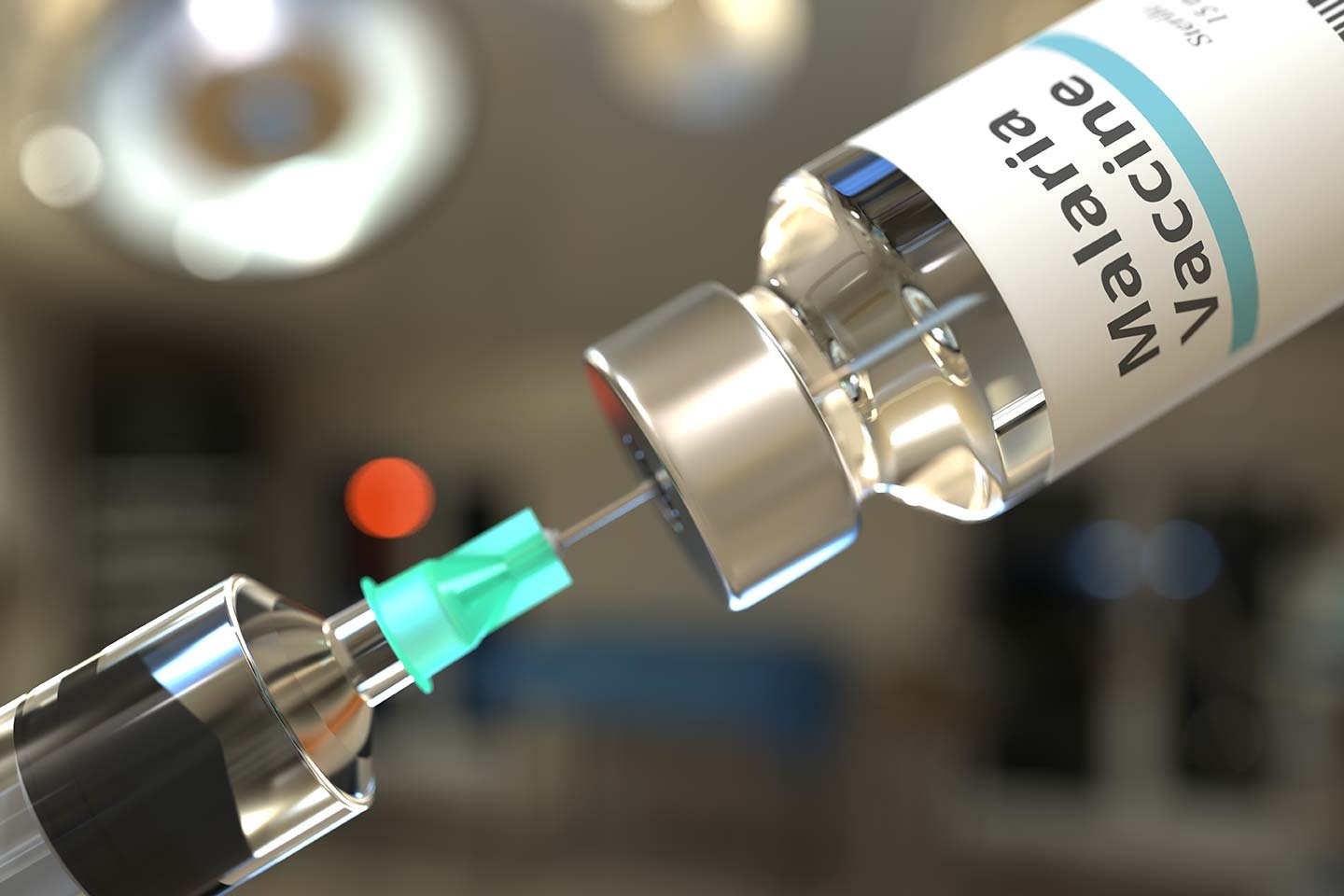
Malaria remains one of Uganda’s most pressing public health challenges, significantly contributing to high morbidity and mortality rates, especially among young children. With the planned introduction of the malaria vaccine in April 2025, the Ugandan government aims to alleviate the burden of this life-threatening disease. This article outlines key aspects of the malaria vaccine, including its benefits, safety, and the implementation strategy for a smooth rollout.
Current Malaria Situation in Uganda
Malaria is the leading cause of illness and death in Uganda, affecting thousands of people daily. According to the 2024 Health Management Information System (HMIS) report:
- 32,900 people contract malaria every day, disrupting daily activities.
- 16 deaths occur daily due to malaria, a preventable disease.
- 6,500 children become ill from malaria each day, with 10 succumbing to the disease.
- Treating malaria costs families an estimated UGX 15,000 per episode, which is a significant financial burden.
- Uganda accounts for 4.8% of global malaria cases, with 12.6 million cases reported in 2023.
Introduction of the Malaria Vaccine
The malaria vaccine will be integrated into Uganda’s routine immunization program starting in April 2025. It will be prioritized in districts with moderate to high malaria transmission rates. Key aspects of the rollout include:
- The vaccine will be provided free of charge, funded by the Ugandan government and international partners.
- It will complement, but not replace, other malaria control measures, such as:
- Insecticide-treated bed nets (ITNs)
- Indoor residual spraying (IRS)
- Seasonal and perennial malaria chemoprevention (SMC/PMC)
- Prompt testing and treatment
How the Malaria Vaccine Works
The malaria vaccine stimulates the immune system to prevent the malaria parasite from infecting the liver, stopping the infection from progressing and thereby reducing the risk of severe illness and death.
Benefits of the Malaria Vaccine
The introduction of the vaccine is anticipated to yield significant health and economic benefits, including:
- Preventing 800 cases of severe malaria daily.
- Reducing hospitalizations and deaths among children.
- Saving families UGX 15,000 per treatment that would otherwise be spent on malaria medication and hospital visits.
- Decreasing the national economic burden by saving millions in healthcare costs and boosting productivity.
Safety and Effectiveness
The malaria vaccine has undergone clinical testing involving over 800,000 children in various African countries. It has been successfully used in Ghana, Kenya, Malawi, Cameroon, and South Sudan since 2019. Over 6 million doses have been administered, demonstrating a good safety profile with no serious side effects reported. The vaccine is certified by the World Health Organization (WHO) and approved by the National Drug Authority in Uganda.
Eligibility for the Vaccine
During the rollout phase, all children aged between six to eleven months will be eligible for vaccination. The vaccine will be administered in four doses:
- First dose: At 6 months
- Second dose: At 7 months
- Third dose: At 8 months
- Fourth dose: At 18 months
Complete vaccination is necessary for maximum protection against malaria.
Common Side Effects
The vaccine may cause mild and temporary side effects, including:
- Pain, redness, and swelling at the injection site.
- Mild fever or fatigue.
- In rare cases, fever-induced convulsions, similar to those seen with other childhood vaccines.
Parents and caregivers are advised to seek medical attention if any severe reactions occur.
Availability and Storage
The vaccine will be available at all public and private health facilities that provide routine immunization services. It will be stored at temperatures between +2°C and +8°C to maintain its effectiveness.
Integration with Routine Immunization
Parents are encouraged to take their children for routine immunizations nine times before their second birthday. Health workers will offer guidance to ensure children receive all necessary vaccines on time.
Call to Action
For a successful rollout of the malaria vaccine, all stakeholders have essential roles to play:
- Parents & Caregivers: Ensure children receive all four vaccine doses.
- Community Leaders, Health Workers, Cultural & Religious Leaders: Educate and promote vaccine acceptance.
- Media & Influencers: Share accurate information to counter vaccine misinformation.
- Government & Partners: Ensure sustainable financing and equitable distribution of the vaccine.
- Politicians: Advocate for vaccine uptake and support community sensitization efforts.
The introduction of the malaria vaccine marks a significant milestone in Uganda’s fight against malaria. While the vaccine is not a standalone solution, it serves as a crucial addition to existing prevention strategies. Parents, caregivers, and community leaders must collaborate to ensure all eligible children receive full vaccination for a healthier, malaria-free Uganda.
For more information, contact the Ministry of Health Uganda through their toll-free lines: 0800 100066 / 0800 200 600 or visit www.health.go.ug.
Health
DEI Biopharma’s CRISPR Platform Promises Affordable, Universal Gene Therapy in fight against Sickle Cell Disease.
Ugandan biotech pioneer Dr. Matthias Magoola and DEI Biopharma have unveiled a game-changing CRISPR-based gene therapy platform for sickle cell disease. By targeting a universal genetic switch to reactivate fetal hemoglobin, this standardized approach promises affordable, scalable treatment for all patients; potentially the first “generic” gene therapy for a monogenic disease. A major step toward equitable access in Africa and beyond, especially as Uganda ramps up national SCD prevention efforts.

In a significant advancement for global health equity, DEI Biopharma, a Uganda-based biotechnology firm, has unveiled a pioneering CRISPR-based gene therapy platform for sickle cell disease (SCD). Invented by the company’s founder and CEO, Dr. Matthias Magoola, this innovative approach targets a universal genetic switch to reactivate fetal hemoglobin, offering a scalable and patient-independent solution that could transform access to curative treatments, particularly in resource-limited regions like sub-Saharan Africa.
Sickle cell disease, a genetic blood disorder affecting millions worldwide, disproportionately impacts populations in Africa, where over 75% of global cases occur. In Uganda alone, an estimated 20,000 children are born with SCD each year, with many not surviving past their fifth birthday due to limited access to screening, treatment, and management. Recent initiatives underscore the urgency: In October 2025, Uganda’s Health Minister, Dr. Jane Ruth Aceng, launched the National Sickle Cell Prevention and Management Scale-Up Programme in Lira City, highlighting the Lango region’s highest prevalence based on nationwide surveillance; the first of its kind in Africa. This effort included establishing a National Taskforce for SCD prevention, integrating services into non-communicable disease frameworks, and receiving donations like 20,000 newborn screening kits and hydroxyurea doses from international partners.
Compounding the challenge is the prevalence of the sickle cell trait (SCT), the carrier state that can pass the disease to offspring. A 2022 study among secondary school students in Kampala revealed that 5.8% carried SCT, yet knowledge levels were only moderate, with 60.4% of participants showing basic understanding of screening and inheritance. Attitudes toward testing were largely negative (67%), influenced by fears of stigma, pain, and relationship impacts. Only 1.5% had been previously tested, and factors like knowing a partner’s status or religious affiliation (e.g., Anglicans were twice as likely to screen) played key roles in uptake. The study emphasized the need for comprehensive health education targeting adolescents to boost screening and prevent new cases, aligning with Uganda’s push for institutionalized SCD services.
Against this backdrop, DEI Biopharma’s platform emerges as a game-changer, addressing not just the biological underpinnings of SCD but also the systemic barriers to equitable care.
Traditional gene therapies for SCD often focus on correcting the specific HBB gene mutation responsible for the sickle-shaped red blood cells that cause pain crises, organ damage, and reduced life expectancy. These methods require personalized designs or donor matching, driving up costs and limiting scalability, issues acutely felt in low- and middle-income countries where infrastructure for advanced treatments is scarce.
DEI Biopharma’s CRISPR platform shifts the paradigm by targeting a conserved enhancer of the BCL11A gene, a master regulator that suppresses fetal hemoglobin (HbF) production after birth. By editing this regulatory element, the therapy reactivates HbF, which inhibits the polymerization of sickle hemoglobin and ameliorates symptoms across all SCD genotypes, including HbSS, HbSC, and HbS/β-thalassemia. This “universal genetic switch” eliminates the need for mutation-specific interventions, allowing for a single, standardized product applicable to any patient.
“This invention was designed from the beginning to solve not only the biology of sickle cell disease, but also the access problem,” said Dr. Matthias Magoola. “By targeting a universal genetic switch rather than the sickle mutation itself, we can manufacture a single, standardized gene-editing product applicable to all patients. This opens the door to what we believe can become the first scalable, first-in-line generic gene therapy platform for a monogenic disease.”
Key advantages include:
- Patient Independence: The therapy edits a non-variable DNA sequence shared by all humans, bypassing the need for individualized guide RNAs or donor cells.
- Scalable Manufacturing: Standardized production and quality control reduce costs, supporting both ex vivo (cell-based) and in vivo (direct body) delivery methods.
- Broad Applicability: Effective regardless of the patient’s specific mutation, making it suitable for diverse populations.
This model draws parallels to generic drugs, where once regulatory exclusivities expire, the same composition can be produced at scale and distributed affordably. DEI Biopharma envisions this as a “new category of standardized, reproducible gene-editing therapeutics,” potentially democratizing access in regions like Uganda, where SCD surveillance and screening programs are expanding but curative options remain out of reach.
The platform is protected by a comprehensive patent covering CRISPR compositions, guide RNAs, delivery systems, and therapeutic methods. Preclinical work is underway, evaluating editing efficiency, HbF induction durability, and safety in biological models. DEI Biopharma plans strategic partnerships, regulatory engagements, and phased clinical trials adhering to international standards.
“Sickle cell disease disproportionately affects populations that have historically been last to benefit from medical innovation,” Magoola added. “Our objective is to change that equation by making advanced gene therapy manufacturable, distributable, and affordable at global scale.”
This breakthrough aligns with Uganda’s national efforts, such as the integration of SCD into health systems and calls for community mobilization. By enhancing HbF levels, the therapy could reduce disease severity, complementing preventive measures like newborn screening and genetic counseling. The Kampala study highlighted that while 85% of students wanted to know their status and 88.5% supported testing, barriers like cost and stigma persist; challenges that affordable, universal therapies could help overcome.
About DEI Biopharma
Founded by Dr. Matthias Magoola, DEI Biopharma is dedicated to high-impact, affordable therapies for unmet needs. With a focus on vaccines, biologics, and gene-based medicines, the company leverages innovative science and global partnerships to bridge access gaps in underserved markets.
As Uganda leads Africa in SCD surveillance and prevention, innovations like DEI Biopharma’s platform offer hope for a future where this debilitating disease is not just managed but cured equitably. By addressing both scientific and socioeconomic hurdles, this development could mark a turning point in the global fight against SCD.
Health
Doomscrolling Should Be Considered a Mental Disorder: Lessons from Uganda’s 2026 Elections
In the lead-up to and aftermath of Uganda’s January 15, 2026, general elections, social media platforms like X (formerly Twitter), Facebook, TikTok, and others turned into battlegrounds of intense negativity. Phrases such as “Protect the gains,” “Uganda is Bleeding,” “New Uganda,” and dire warnings of impending collapse dominated feeds.

In the lead-up to and aftermath of Uganda’s January 15, 2026, general elections, social media platforms like X (formerly Twitter), Facebook, TikTok, and others turned into battlegrounds of intense negativity. Phrases such as “Protect the gains,” “Uganda is Bleeding,” “New Uganda,” and dire warnings of impending collapse dominated feeds. Videos showed opposition leaders like Robert Kyagulanyi (Bobi Wine) confronting police, claims of uncontrollable bloodshed, election malpractices, and predictions that the country stood on the brink unless specific leaders took power. Allegedly paid activists, bots, and fervent supporters from both opposition and ruling party sides amplified these narratives, pushing endless streams of alarming content. Scrolling through it all became addictive; each refresh delivered more outrage, fear, or confirmation of bias leaving many Ugandans angry, exhausted, and emotionally drained.
If you found yourself wrapped up in this cycle, reacting impulsively with heated comments, staying up late to “stay informed,” or feeling constant tension regardless of your political side, you were likely doomscrolling. This behavior, far from harmless, exhibits the traits of a compulsive disorder and should be recognized as a form of mental illness.
Doomscrolling is the compulsive habit of endlessly scrolling through feeds saturated with crises, disasters, political outrage, violence, and apocalyptic predictions. What starts as a genuine effort to follow important events spirals into hours of consumption that heightens anxiety, hopelessness, and fatigue. In Uganda’s recent electoral context, the algorithmic push toward emotionally charged content like videos of confrontations, inflammatory claims, and polarized debates made it especially potent. Platforms reward high-engagement negativity, so feeds flooded with stories of “bloodshed,” rigged processes, or national collapse kept users hooked.
The compulsion is evident in the loss of control many experience. People know the content is harmful yet promise themselves “just one more post” before continuing far longer. This mirrors addiction patterns: each alarming update triggers a dopamine hit from novelty or perceived threat awareness, an ancient survival instinct distorted by infinite digital feeds. Tolerance develops quickly, more extreme content is needed for the same “informed” feeling while stopping brings restlessness or fear of missing critical updates.
Psychological research from recent years, including studies in journals like Computers in Human Behavior, links doomscrolling to serious mental health impacts stating that “Media and media content overload can serve as a conduit for mental health problems, such as anxiety and depression”. “The media facilitates accessibility to specific thoughts and triggers relevant reactions. For example, exposure to violent media has been shown to implant aggressive thoughts and increase antagonism”.
It heightens psychological distress through poor emotional regulation and problematic social media use. In adults and youth alike, prolonged exposure predicts rises in anxiety, depression, chronic stress, and existential despair; feelings of meaninglessness, deep distrust in others (including fellow citizens), and a bleak worldview. During Uganda’s election period, this manifested as constant anger, sleep disruption from late-night scrolling, elevated cortisol levels, and physical effects like fatigue or high blood pressure. For those with preexisting vulnerabilities, the habit created vicious cycles: negative posts reinforced biased perceptions, fueling more scrolling and deeper emotional lows.
Experts increasingly frame doomscrolling in addiction-like terms, driven by platform designs such as infinite scrolling, notifications, and algorithms that amplify outrage for engagement. It shares mechanisms with conditions like the compulsive Internet Gaming Disorder (IGD-11) noted in the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) and broader problematic social media use. While not yet a standalone diagnosis in manuals like the DSM-5 or ICD-11, severity scales now quantify it as a rigid, harmful behavioral cluster. In politically charged environments like Uganda’s 2026 polls marked by internet blackouts, arrests of unruly opposition radicals, and polarized discourse; the risks intensify, turning information-seeking into a self-perpetuating source of suffering.
The argument for classifying it as mental illness is clear: when a behavior is compulsive, dopamine-driven, resistant to simple willpower, and consistently linked to psychiatric worsening including exacerbated depression, generalized anxiety, insomnia, reduced life satisfaction, and even physical health decline, it enters pathological territory. Dismissing it as “just keeping up with politics” ignores the toll on millions, especially in high-stakes contexts where social media becomes the primary source of news amid restrictions.
Formal recognition would enable better responses. Mental health professionals could screen for doomscrolling in clients showing anxiety, low mood, or sleep issues, using cognitive-behavioral techniques to break reward loops, build uncertainty tolerance, and foster healthier habits. Public campaigns in Uganda and beyond could highlight it alongside other compulsions, urging balanced consumption. Platforms might add tools like scroll limits or negativity filters which is very highly unlikely, though history shows governments sometimes restrict access instead. Individually, enforce device curfews, designate no-news periods, curate positive or neutral follows, and practice mindfulness to sit with uncertainty rather than chase endless updates.
Doomscrolling during Uganda’s 2026 elections was not mere curiosity, it was a digital trap eroding mental well-being amid real political tensions. Viewing it as a form of mental illness is not alarmist; it is a vital acknowledgment that helps us reclaim agency in an era engineered to keep us scrolling through the shadows. By naming the problem, we take the first step toward healthier engagement with our shared reality.
Health
Uganda’s 2025 Ebola-Free Victory, Resilience and Global Prevention Lessons
Uganda was officially declared Ebola-free, marking the end of its sixth Ebola outbreak in just under three months.

Uganda was officially declared Ebola-free, marking the end of its sixth Ebola outbreak in just under three months. The outbreak, caused by the Sudan strain of the Ebola virus, began on January 29, 2025, in Kampala and affected five districts, resulting in 14 confirmed cases and four deaths. Uganda’s swift containment of this urban outbreak, despite challenges such as international aid cuts and the absence of approved vaccines, demonstrates a robust public health response and offers critical lessons for global Ebola prevention.
The outbreak was declared on January 29-30, 2025, after a 32-year-old male nurse died at Mulago National Referral Hospital in Kampala. The virus was confirmed as Sudan Ebola Virus Disease (SUDV) by three national laboratories and was genetically linked to a 2012 outbreak in Luwero, Uganda. Unlike the Zaire strain, which has an approved vaccine, the Sudan strain lacks licensed countermeasures, making containment reliant on public health measures and experimental trials. The outbreak spread to five districts being Kampala, Wakiso, Jinja, Mbale, and one other, posing a significant threat due to Kampala’s dense population of over 4 million. By February 7, 2025, new cases ceased, and the last patient was discharged on March 14, initiating a 42-day countdown. On April 26-28, 2025, Uganda’s Ministry of Health announced the end of the outbreak, a testament to the country’s experience with five prior Ebola outbreaks since 2000.
Uganda’s ability to contain the 2025 outbreak in under three months, its shortest Ebola response to date, was driven by a multi-faceted strategy:
Rapid Detection and Genomic Sequencing
Within 24 hours of the index case’s death, Uganda’s Central Public Health Laboratories confirmed the Sudan strain, and African scientists set a “world speed record” by sequencing the virus, tracing its origins back to the 2012 outbreak. This rapid diagnostic and genomic capability enabled an immediate outbreak declaration on January 30, 2025, activating emergency protocols.
Aggressive Contact Tracing and Quarantine
The Ministry of Health identified 265 contacts of the index case, placing them under strict 21-day quarantine in Kampala, Jinja, and Mbale. Mobile health teams and district task forces monitored contacts daily, preventing further spread. A surveillance gap, exposed when a four-year-old boy died undiagnosed on February 25, was swiftly addressed by intensifying tracing, adding two districts to the response. By February 27, most contacts had completed their quarantine.
Experimental Vaccine Trial
On February 3, 2025, Uganda launched a randomized clinical trial for a candidate SUDV vaccine at Mulago Hospital, using a ring vaccination approach to immunize contacts and contacts-of-contacts. Supported by the International AIDS Vaccine Initiative and WHO, the trial drew on lessons from the 2022 outbreak, demonstrating Uganda’s ability to integrate research into crisis response.
Isolation and Treatment
Confirmed cases were isolated at Mulago Hospital, with suspected cases triaged in temporary units. Supportive care, including rehydration and symptom management, was critical, as no approved SUDV treatments exist. Eight patients were discharged by February 19, and the last patient on March 14, with safe burial practices preventing transmission from the four deaths (two confirmed and two probable).
Public Health Measures
Uganda implemented point-of-entry and exit screenings at airports and borders, which were crucial given Kampala’s role as a transport hub. Community awareness campaigns via radio and local leaders educated the public on Ebola symptoms and prevention, countering misinformation. Healthcare workers used personal protective equipment (PPE), though supply shortages resulting from U.S. aid cuts were mitigated by WHO and local resources.
International and Local Collaboration
Local expertise was evident in Uganda’s laboratories and the Uganda Virus Research Institute, which supported diagnostics and trials. Internationally, the U.S. provided $8 million via the CDC and USAID, despite aid cuts that canceled four contracts, impacting screenings and PPE supplies. The WHO contributed $2 million and technical expertise, while the UN appealed for $11.2 million to support seven high-risk districts. Uganda shared genomic data regionally, aiding preparedness amid Marburg outbreaks in Tanzania and Rwanda.
Urban Setting: Kampala’s high population density risked rapid spread, but targeted interventions in five districts prevented a wider epidemic.
Aid Cuts: The Trump administration’s freeze on USAID funding strained surveillance and PPE supplies, but local and WHO support helped offset this shortfall.
Surveillance Gaps: The delayed diagnosis of a child emphasized the need for improved surveillance, which was quickly addressed through intensified efforts.
By overcoming these challenges, Uganda showcased resilience and innovation in its public health response, setting an example for global health efforts against Ebola and similar infectious diseases.
-

 Entertainment1 year ago
Entertainment1 year agoMuseveni’s 2025 Copyright for Musicians breakdown
-

 Business1 year ago
Business1 year agoUganda’s Ministry of Finance projects significant growth opportunities in 2025
-

 Business1 year ago
Business1 year agoThe 9 worst mistakes you can ever make at work
-

 Policies1 year ago
Policies1 year agoBreakdown of the Uganda Police Force Annual Crime Report 2024
-

 Sports1 year ago
Sports1 year agoThe Transformative Impact of World Cup Qualification for Uganda
-

 Policies1 year ago
Policies1 year agoIs Uganda’s Shs10m Fine the WORST Thing for Cohabiting Couples?
-

 Health1 year ago
Health1 year agoThe Nutritional Benefits of Maize Flour (Posho)
-

 Entertainment1 year ago
Entertainment1 year agoIsaiah Misanvu Teams Up with Nil Empire for a Soul-Stirring Anthem of Gratitude and Transformation “Far Away”